"Coffee smells like something rotten" | Post-COVID parosmia, the brain's desperate signal


"The coffee my husband brought me smells like a drain.
The doenjang jjigae I used to love now makes me feel nauseous.
I'm afraid I'm going crazy, or that something is seriously wrong with my brain — I can't sleep every night from the fear."
These were the first words of Su-jin (pseudonym), a worker in her 40s, who came to my clinic complaining of parosmia after COVID infection.
For Su-jin, who had always enjoyed cooking and loved cafes, the world of smells had completely flipped — about 3 weeks after being declared recovered.
At first she waited, thinking it would be temporary aftereffects, but two months later the symptoms were unchanged.
The ENT said there was no abnormality on olfactory nerve tests; neurology also returned a normal MRI result.
When she said "Tests are all normal — so why am I like this?", her voice carried a loneliness deeper than pain.
The helplessness of suffering something clearly real that no one could explain — I couldn't help but feel heavy inside.
I did not see Su-jin's symptoms as simply a peripheral nerve malfunction.
So why, after COVID, are some smells distorted, while others disappear entirely?
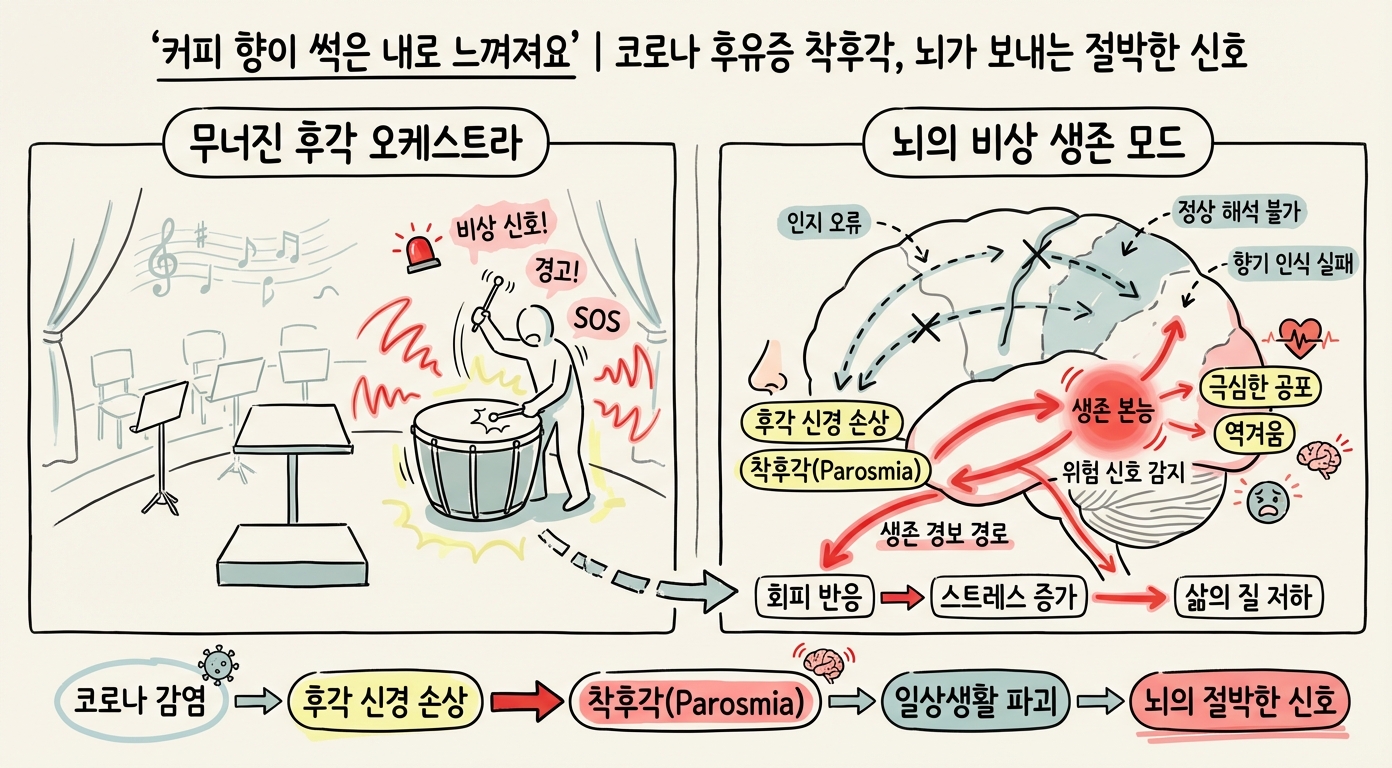 The Broken Orchestra and the Wailing Percussion: What Happens Inside the Brain
The Broken Orchestra and the Wailing Percussion: What Happens Inside the Brain
The olfactory sense is the only one among the five human senses that connects directly deep into the brain without passing through the thalamus — a special pathway.
This signal is then processed by the brain along two major branches.
The first is the primitive survival pathway (amygdala · hypothalamus).
This is the primary defense system that immediately detects life-threatening smells — such as rotting food or toxic chemicals — and triggers an avoidance response.
The second is the higher-order cognitive and memory pathway (hippocampus · orbitofrontal cortex).
This is the sophisticated system that cross-references past memory data to read delicate fragrances entangled with memory and emotion — the smell of childhood, the flavor of favorite foods, a loved one's perfume.
Normally these two pathways work harmoniously together, like an orchestra, helping us experience the world's smells richly.
Post-COVID parosmia begins precisely when the balance of this orchestra collapses.
When the aftermath of infection leaves micro-neuroinflammation around the olfactory bulb and in higher-order processing areas such as the orbitofrontal cortex, or reduces network connectivity there, the function of decoding delicate fragrances in tandem with memory is the first to shut down.
On the other hand, the primitive alarm pathway directly connected to survival survives almost undamaged.
Without the normal cognitive filter working, instead of interpreting incomplete incoming signals positively, the brain assumes the worst — decay or toxic substances — and continuously sends out warning signals.
It is like a percussion player alone, furiously beating an emergency signal in an orchestra whose conductor and string section have all left the stage.
Su-jin's coffee smelling like a drain was not her brain breaking down.
In a state where higher-order cognitive function was blocked, her brain was running olfaction in emergency survival mode — to protect her.
Then why can the brain not turn off emergency mode for so long?
There are reasons beyond simple nerve damage for parosmia continuing for months.
In Korean medicine, COVID is seen as 온독 (瘟毒) — an external pathogen (外邪) with the character of intense heat-toxin.
When this heat-toxin directly invades the lung (肺), 폐기 (肺氣) — the lung's power to coordinate sensory perception through the nose — weakens.
심신 (心神) — which integrates and stabilizes sensory information — is destabilized, and 신정 (腎精) — the source that fills the brain marrow — is deeply consumed.
When these three overlap, the brain's overall sensory coordination capacity falls and the amygdala's hyperactivation persists for a long time.
There are also things you can try on your own.
Twice a day, slowly and with concentration smelling four familiar fragrances vivid in memory — calling to mind the memories connected to each — is a form of olfactory retraining that research supports as stimulating neuroplasticity.
Strong, clear fragrances such as rose, lemon, clove, and eucalyptus are well-suited for training.
From the Korean medicine perspective, treatment that simultaneously supplements depleted 폐기 (肺氣) and 심신 (心神) while gradually driving out the residue of lurking heat-toxin helps create conditions for the brain to once again run both pathways in balance.
However: if parosmia is accompanied by severe headache, speech difficulty, visual disturbance, or weakness in one arm or leg, this may be a neurological emergency beyond ordinary COVID aftereffects — seek a neurological specialist without delay.
 From Emergency Mode to Daily Mode: Your Brain Is Still on Your Side
From Emergency Mode to Daily Mode: Your Brain Is Still on Your Side
Recovery from parosmia is not fast.
Building new pathways in the brain's neural network requires time and repetition.
Please take a moment to listen quietly to what these confusing signals your body is sending you.
Your brain has not broken down.
In the shock of infection, it has simply been standing guard alone for far too long — to protect you.
If we find the right direction together, the brain will surely find again the day when it remembers coffee as coffee, and flowers as flowers.
Not simply suppressing symptoms, but looking again at the whole collapsed sensory environment and restoring it — that is the direction of treatment I aim for.
My role is simply to be a small companion by the patient's side on that journey of recovery.
Even if not with me — please find a healthcare provider who truly empathizes with your suffering and can attend with care to the most subtle imbalances of the body as a whole.
Please do not endure the loneliness of those unfamiliar smells alone.
Reviewed by Director Jang-hyeok Choi, Dongjedang Korean Medicine Clinic


